SARAH REINGEWIRTZ/MEDIANEWS GROUP/LOS ANGELES DAILY NEWS VIA GETTY IMAGES
Monkeypox cases are plummeting. Scientists are debating why
Models suggests rising immunity in a small group of people with many sexual contacts is key
26 OCT 2022 11:35 AM. BY KAI KUPFERSCHMIDT
When monkeypox cases in Europe began to decline this summer, researchers’ first question was: Is it real? Some worried that people might not be getting tested because of receding fears of the virus, coupled with strict isolation requirements for patients. “They might be reluctant to be confirmed and be told not to go out at all,” says Catherine Smallwood, monkeypox incident manager at the World Health Organization’s (WHO’s) Regional Office for Europe.
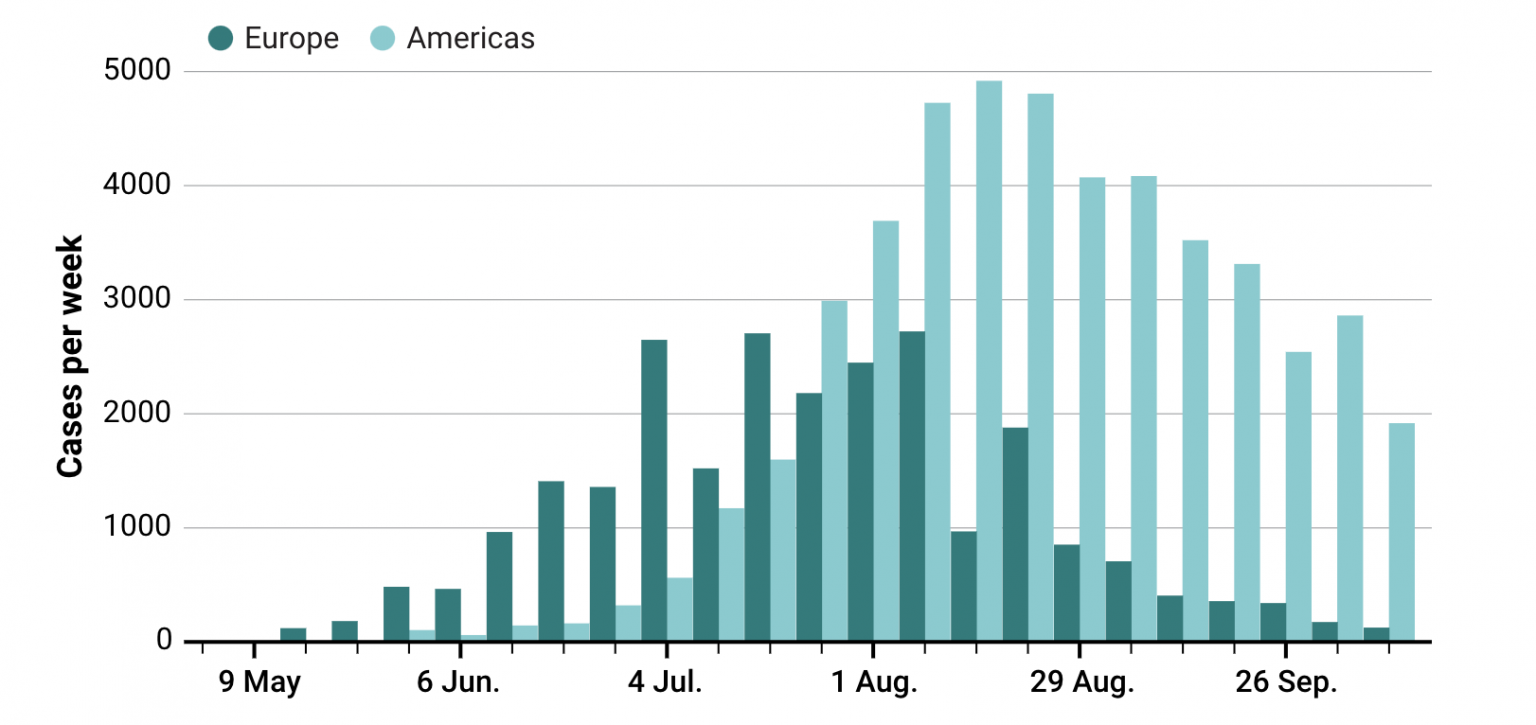
But the decline is now unmistakable. WHO Europe, which reported more than 2000 cases per week during the peak in July, is now counting about 100 cases weekly. In the Americas, the other major epicenter of the outbreak, numbers have dropped by more than half (see graphic, right). “We’re seeing a true decline,” Smallwood says.
Vaccines, behavior change among the most affected group—men who have sex with men (MSM)—and immunity after natural infection are all playing a role in that decline, says Erik Volz, an infectious disease modeler at Imperial College London, but how much each factor has contributed is unclear. “This is something we’ve debated a lot internally.”
The answer is important because it determines the likelihood of a resurgence of the virus. Knowing what has driven down cases so far will also help shape strategies to eliminate the virus outside endemic countries in Africa, a goal WHO Europe is already pushing for.
Immunity acquired through infections in the most sexually active men may be the biggest factor, however. Monkeypox has been affecting mostly MSM and their sexual networks because parts of those networks are densely connected, with some people having a large number of sexual contacts. Rising immunity in that group could limit the viru’s ability to spread, says Jacco Wallinga, chief epidemic modeler at the Dutch National Institute for Public Health and the Environment. “Because the persons with a very high number of sexual contacts are also those at the highest risk of infection, the depletion of susceptibles due to natural infection is very rapid,” he says. Brand agrees. His model suggests that among the estimated 1000 people in the United Kingdom who have 120 sexual partners per month or more, “maybe half got infected by the time of the peak.” Still, Brand says his model suggests infections among this small part of the MSM population cannot explain the observed decline on their own. “I don’t think it is as plausible” as behavior change playing a role as well, he says.
In the United Kingdom, at least, vaccination campaigns have played a minor role, according to a model published as a preprint this month by Samuel Brand, an infectious disease modeler at the University of Warwick. Monkeypox’s reproductive number—the average number of new infections triggered by an infected person—began to drop by mid-June, even though campaigns only started in July, Brand notes. Several other European countries saw the same pattern.
That leaves behavior change and immunity from natural infections. A survey conducted by the U.S. Centers for Disease Control and Prevention among MSM in August found about half had reduced their number of sexual contacts. As awareness of the disease increased, people also became more likely to seek diagnosis and treatment early and to avoid sex while they were infectious. The UK Health Security Agency has presented data suggesting syphilis and other sexually transmitted infections declined as well—which would bolster the case for behavior change—although that signal is “suggestive but not conclusive,” Volz says.
Passing waves
The two hardest hit World Health Organization regions—Europe and the Americas—are both seeing a steep decline in monkeypox cases.
GRAPHIC: K. FRANKLIN/SCIENCE; DATA: WORLD HEALTH ORGANIZATION
For Smallwood, that raises a concern: that MSM who feel reassured by the plummeting case numbers may revert to their past behavior. That’s why vaccination of at-risk groups may now be more important than it was at the peak of the epidemic, she says. Brand agrees; in fact, his U.K. model suggests that although a slight uptick in cases in the coming months is likely, vaccinations should prevent a real resurgence. “I don’t think there’s room for complacency at this point,” he says.
Eliminating the virus altogether from nonendemic countries may be difficult. “That last bit is always the hardest,” Smallwood says. Among the reasons are stigma and discrimination. “In many countries, [infected people] will not be presenting purely because they’re concerned about how they may be treated,” she says. Besides, it has become clear that some people have asymptomatic infections and could pass on the virus unknowingly, says Boghuma Titanji, a virologist at Emory University.
Even if, say, Europe or the United States managed to eliminate the virus, reintroductions from sexual networks in countries where the virus is still circulating in humans would remain a threat, Smallwood says. And the ultimate source of the virus will remain untouched: the animal species in Africa where the virus circulates, occasionally spilling over to humans, as it has for decades. “This is not an outbreak that just needs to be fixed, and then the risk is gone,” Smallwood says.
https://www.science.org/content/article/monkeypox-cases-are-plummeting-scientists-are-debating-why